Files
Download Full Text (1.1 MB)
Description
Acute rashes vary widely in presentation and severity, with many being mild while others like Stevens-Johnson Syndrome (SJS) are true dermatologic emergencies. Rashes can have a variety of causes, including drugs, infection, and autoimmune disorders. While supportive care is a mainstay of all acute rashes, differentiating types of reactions can allow for more directed treatment, and in the case of multifactorial skin pathologies, can help determine how different factors affect presentation. We present a case of acute rash initially concerning for SJS but found to have multifactorial contributions due to a complex clinical course. The patient is a 74 y.o. female with a history of paroxysmal Afib, COPD, DVT, and diastolic heart failure who presented to an outside hospital after a fall. As an outpatient she had received separate courses azithromycin and doxycycline for bronchitis.
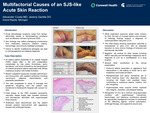
She was found to be hypotensive and hypothermic and was admitted to the ICU. Due to left leg swelling and history of DVT, CT was obtained and found an extensive left iliac vein DVT and reduced caliber of the IVC. A pelvic hematoma was also observed, likely related to her fall. She completed thrombectomy and continued on IV heparin. She had a complex ICU course with worsening of the hematoma requiring multiple transfusions and increasing pressor requirements along with abdominal pain, fever, and rash. Erythema and warmth were noted on the lower abdomen, buttocks, groin, and bilateral lower extremities. Oral lesions were not noted. Abdominal CT showed acute pancreatitis with complex fluid collection and stable pelvic hematoma. She received vancomycin, cefepime, metronidazole, and piperacillin-tazobactam during the admission. She transferred to the floor and was noted to have significant lower extremity edema due to extensive fluid resuscitation in the ICU.
In contrast, this patient lacked mucosal erosions and had multiple contributors to her dermatitis in addition to antibiotic exposure. Her pelvic hematoma led to extravasation of blood that migrated to dependent areas that correlated to the most severe wounds. She also had edema from fluid resuscitation and a superimposed fungal infection. The multifactorial nature of her dermatitis required a varied treatment approach, with diuresis and antifungals playing roles that would not have existed if SJS were the primary diagnosis.
Publication Date
5-8-2026
Disciplines
Internal Medicine
Recommended Citation
Cooke A. Multifactorial causes of an SJS-like acute skin reaction. Presented at: Research Day Corewell Health West; 2026 May 8; Grand Rapids, MI.

Comments
2026 Research Day Corewell Health West, Grand Rapids, MI, May 8, 2026. Abstract 2066