Files
Download Full Text (682 KB)
Description
Pityriasis lichenoides et varioliformis acuta (PLEVA) is a group of inflammatory skin disorders. Febrile Ulceronecrotic Mucha-Habermann disease (FUMHD) represents a subtype with rapidly progressive necrotic papules that evolve into painful, coalescent ulcers with hemorrhagic crusts, bullae, and pustules [1]. Systemic manifestations include high fever, sore throat, diarrhea, central nervous system symptoms, abdominal pain, interstitial pneumonitis, splenomegaly, arthritis, sepsis, megaloblastic anemia, conjunctival ulcers, and death [2]. Hemophagocytic lymphohistiocytosis (HLH) is an immune activation syndrome causing prolonged fever, hepatosplenomegaly, cytopenias, and elevated markers of inflammation [3]. FUMHD-associated HLH is extremely rare and only a handful of cases have been reported to date [4]. This is a case of an HLH flare triggered by underlying FUMHD.
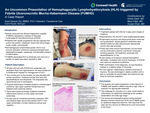
The patient is a 48-year-old man with PLEVA who presented with persistent fever and hyponatremia. He was transferred to Butterworth hospital in Grand Rapids, Michigan for management of HLH. Two months prior to the transfer, he was admitted with similar symptoms and met HLH criteria. At the time, treatment was started with dexamethasone and etoposide. The etoposide was discontinued due to neutropenia. At the time of admission, he had fatigue and lethargy but was alert and oriented. Vital signs were unremarkable except for fever and tachycardia. Physical examination revealed posterior oropharyngeal erythema, right upper quadrant tenderness and bilateral lower extremity edema. There were partial thickness scattered ulcerative inflammatory lesions on both upper and lower extremities. He also had an incidental pulmonary embolism (PE) and bilateral deep venous thrombosis (DVT) in the upper extremities. A broad infectious workup was negative.
The severity and rapid progression of skin lesions in FUMHD with systemic effects requires a high index of suspicion for appropriate treatment. The challenge for clinicians is in rarity, which leads to unfamiliarity. An additional challenge is the variable presentation and wide age range. The clinical and histopathological overlap between Stevens-Johnson Syndrome (SJS) and FUMHD poses an additional diagnostic dilemma [5]. We hope that this case can be a source of reference for such encounters in the future.
Publication Date
5-8-2026
Disciplines
Internal Medicine
Recommended Citation
Zia S, Qadir S, Khan A, Patel M. An uncommon presentation of hemophagocytic lymphohistiocytosis (HLH) triggered by febrile ulceronecrotic Mucha-Habermann disease (FUMHD): A case report. Presented at: Research Day Corewell Health West; 2026 May 8; Grand Rapids, MI.

Comments
2026 Research Day Corewell Health West, Grand Rapids, MI, May 8, 2026. Abstract 2077