Files
Download Full Text (293 KB)
Description
Herpes simplex virus (HSV) encephalitis is the leading cause of sporadic viral encephalitis and remains associated with substantial morbidity despite appropriate antiviral therapy. Increasing data support a secondary immune-mediated encephalitis occurring after HSV infection, most commonly associated with antibodies against the N-methyl-D-aspartate receptor (NMDA-R). This post-infectious process is uncommon and frequently underrecognized, particularly in adults, creating a diagnostic gap when patients develop delayed neurologic deterioration after apparent virologic resolution. Failure to identify this biphasic disease course can result in delayed immunotherapy and prolonged neurologic injury.
We present a detailed case report of autoimmune NMDA-R encephalitis following HSV encephalitis. Clinical data were obtained through comprehensive chart review, including neurologic examinations, serial neuroimaging, cerebrospinal fluid (CSF) analyses, electroencephalography, and treatment response. Diagnostic reassessment focused on predefined clinical inflection points, including recurrent encephalopathy and inflammatory CSF profiles, prompting evaluation for secondary autoimmune encephalitis. A focused review of contemporary literature was performed to contextualize diagnostic and therapeutic decision-making.
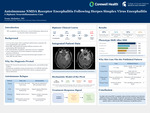
A 66-year-old female presented with acute encephalopathy and confusion. Brain MRI demonstrated asymmetric diffusion restriction with corresponding ADC hypointensity in the inferior medial left temporal lobe. CSF analysis confirmed HSV encephalitis, and she completed intravenous acyclovir therapy. Her course was complicated by focal status epilepticus requiring multiple antiseizure medications. Despite virologic treatment and seizure control, she developed progressive cognitive and functional decline approximately 4 weeks later, representing a critical clinical inflection point described in post-HSV autoimmune encephalitis cohorts (Armangue et al., 2015; Prüss et al., 2018). Repeat CSF demonstrated elevated protein, mild pleocytosis, and intrathecal IgG synthesis. Autoimmune encephalitis testing returned positive for NMDA-R antibodies, establishing the diagnosis. She was treated with high-dose intravenous methylprednisolone followed by plasma exchange, resulting in clinical stabilization, consistent with report
This case highlights a critical diagnostic gap in the evaluation of delayed encephalopathy following HSV encephalitis. Recognition of clinical inflection points and early consideration of autoimmune mechanisms are essential to avoid misattribution to viral relapse or seizure-related encephalopathy. Contemporary evidence supports early immunotherapy to improve neurologic outcomes (Graus et al., 2016; Abboud et al., 2023). Increased awareness of post-HSV NMDA-R encephalitis is necessary to refine diagnostic pathways and optimize patient care.
Publication Date
5-8-2026
Disciplines
Neurology
Recommended Citation
Abobaker E, McCarthy P. Post-HSV NMDAR encephalitis: A case of biphasic neuroinflammation. Presented at: Research Day Corewell Health West; 2026 May 8; Grand Rapids, MI.

Comments
2026 Research Day Corewell Health West, Grand Rapids, MI, May 8, 2026. Abstract 2090