Files
Download Full Text (205 KB)
Description
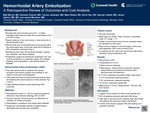
Limited options exist for hemorrhoidal disease in patients with severe comorbidities such extreme frailty, chronic pain, cirrhosis, or the need for continuous anti-coagulation. Hemorrhoidal artery embolization (HAE) has been proposed as a less invasive modality for treatment of patients who are unable to undergo banding or excision due to surgical contraindications, however data is limited. Our primary aim was to assess the efficacy of HAE compared to rates of recurrence and complications at a tertiary referral center to better understand which patients are most likely to benefit. Our secondary aim was to characterize charges associated with the procedure.
A retrospective review was performed on all patients referred for HAE to an Interventional Radiology department from 2020 - 2025. The primary outcome was clinical success, defined as resolution of hemorrhoidal bleeding, not requiring additional procedures. Data regarding demographics, clinical indication, pre- and post-procedural clinical status, outcomes, charges associated with the encounter, and the need for further hemorrhoid-related procedures were collected.
We identified 55 patients who underwent 69 instances of HAE. There were 26 female patients and 29 males with 35% (n=19) with grade 2 hemorrhoids. Mean age was 66, and mean Charlson-Comorbidity Index was 4.7 (range 1-11, mode 3). The most common surgical contraindication was continuous anticoagulation (58%, n = 32), followed by cirrhosis (22%, n = 12). Resolution of bleeding occurred after initial HAE in 62% of patients, however, 40% experienced hemorrhoidal recurrence. A second embolization was attempted in 13 cases, with clinical success achieved after one additional procedure in 62% (n = 8). Out of the 55 patients, 14.5% underwent additional procedures with colorectal surgery, most commonly excisional hemorrhoidectomy (n = 6). Two patients underwent banding and one is undergoing serial anal dilations. The average charges per HAE event was $17,574 (range $5,542 - 70,919).
Our results demonstrate that HAE is a safe option for patients with significant co-morbidities. In terms of resolution of bleeding, HAE was successful in most patients, however the procedure is also associated with significant rates of recurrence and need for repeat procedures. Future studies will be necessary to understand if this recurrence rate outweighs the risk associated with surgical intervention, as 15% of subjects still underwent surgery in this cohort. Additional studies can also compare charges incurred to traditional non-surgical options, such as sclerotherpies.
Publication Date
5-8-2026
Disciplines
Surgery
Recommended Citation
Morris M, Cadoret D, Jahangiri Y, Liefeld H, Han H, Ogilvie Jr. J, Morrison J. Hemorrhoidal artery embolization: A retrospective review of outcomes and cost analysis. Presented at: Research Day Corewell Health West; 2026 May 8; Grand Rapids, MI.

Comments
2026 Research Day Corewell Health West, Grand Rapids, MI, May 8, 2026. Abstract 1924